When we watch the news, when we see stories of people whose health and lives are in danger, when we read accounts of human suffering, does being a nurse make a difference? Do we bear a special responsibility? A responsibility to “nurse out loud,” to take a stand and speak out?
More and more nurses are looking to the border and saying “yes,” our conscience and professional responsibility compels us to. Especially now at least five children have died in government custody in nine months, we have to call out the inhumane conditions in the detention camps and centers where migrants are being held. Some nurses are even travelling there in person to lend a hand, like the volunteers of the Registered Nurse Response Network (RNRN).

Two of the largest nursing organisations in the United States have now issued formal declarations of protest as well. They chose distinctly different approaches, though. Which (if either) of the two do you agree with more?
“This administration is imprisoning thousands of children”: the NNU is “appalled”
The nurses union National Nurses United (NNU) has been protesting the “inhumane and illegal treatment of Central American migrants” since last year, calling it a “humanitarian and public health crisis”. On June 26, the NNU issued a new statement condemning the “unsanitary, dangerous, and brutal conditions threatening the health and well-being of children and asylum seekers at U.S. federal border detention facilities,” and “calling for an immediate end to holding them in federal custody and for swift reunification with family members”.
“As nurses we are appalled and deeply disturbed,” NNU executive director Bonnie Castillo, RN, said, about conditions in facilities like a Border Patrol station in Clint, TX, where attorneys found that young children were forced to care for toddlers, don’t have enough to eat and drink, often sleep on concrete floors in freezing cages with the lights on 24 hours a day, are rarely allowed to shower, bathe, or wash, and suffer from active lice and flu outbreaks.
Castillo called it “unconscionable.. that this administration is imprisoning thousands of children without even meeting their basic needs of adequate shelter and temperature, food, water, clothing, bedding, hygiene, medical care, and caring, adult supervision”. Declaring those conditions a matter of “abuse and a violation of their human rights,” she declared: “This must end now.”
RNRN volunteers continue to hear stories of horrific conditions of #asylumseekers while detained.
Refugees are coming to our border and they need our help––#nurses don’t turn our backs to those in need. Donate to RNRN today –> https://t.co/JlccsnHeuw pic.twitter.com/iCoKdM28Av
— NationalNursesUnited (@NationalNurses) June 10, 2019
The NNU has a long tradition of ‘nursing out loud,’ taking a broad view of the responsibility of nurses. Like Castillo said at one of the union’s many rallies, “We take an oath of patient advocacy; so for us, as nurses, inaction has never been an option.”
Together with the California Nurses Foundation, it was also the NNU which took the lead in organising the RNRN volunteer missions which took place earlier this year and again last month, deploying “teams of mostly Spanish-speaking nurses and nurse practitioners” to care for migrant and asylum-seeker families who were released from federal detention at the Casa Alitas shelter in Tucson’s Benedictine Monastery. The shelter has since provided care to some 8,000 migrants. Application forms to be deployed as nurse volunteers welcome RNs with an active license in one of the border area states, but warns that they must “be willing to work long hours in difficult physical and emotional conditions”.
“Every single person is sick”: nurse volunteers report back from RNRN missions
The volunteers returned with harrowing stories. “Every single person is sick,” said Jessica Rose, RN. “Virtually every woman, man, and child we treated who had come out of federal detention suffered from some sort of respiratory illness, dehydration, and was very hungry,” confirmed Cathy Kennedy, RN. They saw “cases of chicken pox every week” and worried about the spread of such diseases in the detention facilities. “One bus that came from a San Diego detention center had several very sick children on board, including one with chickenpox, and two small children with fevers over 105 degrees,” said Mallory Carellas, a Registered Nurse from Baltimore. “We have a little girl who came in with Leukemia,” Maria Rojas told KOLD News 13.
Since the Registered Nurse Response Network (RNRN) began sending teams of nurses to Casa Alitas in Tucson, AZ, the shelter has provided care to 8,000 migrants. #NursesWeek #UnionStrong pic.twitter.com/isxw6Ftxoq
— NationalNursesUnited (@NationalNurses) May 11, 2019
The volunteering nurses passed on accounts of migrants who said “they were often not able to take care of basic hygiene needs, such as getting diapers for their children,” which “exacerbated skin rashes and infected wounds”. They recounted testimonies by migrants who “told nurses they had their medications confiscated at the border” or “not allowed to take them while in detention”. One woman, Carellas said, suffered from hyperthyroid and hypertension and was forced to go without her daily medication for days while she was in federal custody. “It was mind boggling… She has the medication, she needs the medication, why can’t she take the medication?”
Rose described the case of a Guatemalan mother who “said she had pleaded to get medical care during the five days she was held in detention, but her complaints were ignored”. When the medical team at the shelter examined her, they immediately sent her to the hospital for emergency surgery on an infected gall bladder. Food rations in the detention centers were inadequate too, Carellas claimed: “They are clearly hungry. It was heartbreaking.” In short, the NNU concluded, migrants are not being “housed, fed, and treated humanely in federal detention”. And nurses like Rojas are determined to help: “[when] we said our nightingale vows it wasn’t just to Americans, it was for everyone”.
“Care is not a partisan issue”: the ANA response
The American Nurses Association (ANA), meanwhile, has taken a more cautious stand. “The reports coming from these detention facilities are unfathomable,” the ANA’s Brooke Trainum and Janet Haebler explained, and are confounded by the fact that some of them “are operated by private corporations”. But “what many do not realize” is that the conditions of border detention facilities are “not new”. Since “many Americans are split” on how or whether immigration laws should be reviewed, they clarified, ANA will focus “on the immediate issue of a humanitarian crisis … at the border”.
Last week, the Membership Assembly voted overwhelmingly to express its concern to the Dept. of Homeland Security and Customs & Border Protection regarding the conditions and treatment of #migrant families at the border. Read @ANAPresident's response: https://t.co/QxxfDtd7CT pic.twitter.com/nlLSSJYihK
— American Nurses Association (@ANANursingWorld) June 27, 2019
Nevertheless, the organization’s Membership Assembly pressed for more action. Last June, it “voted overwhelmingly to express its displeasure and utmost concern … regarding the conditions and treatment of migrant families at the border,” ANA President Ernest J. Grant informed the Department of Homeland Security. He called for immediate action “to ensure that immigrant detainees have access to basic hygiene needs, appropriate health care, including mental health care services, and adequate sleeping arrangements”.
Taking care to emphasize that “care is not a partisan issue,” but a human rights issue “bolstered by the resolve of the American people to treat others with compassion,” the ANA implored “the federal government and U.S. Congress to come together” to ensure migrants will receive “basic health care …, safe and sanitary conditions, and policies that allow families to stay together”. It also proposed appointing “an expert task force that includes nurses, especially those who focus in pediatrics and diverse communities”.

Other nursing organisations have weighed in as well. The Public Health Nursing Section of the American Public Health Association (APHAPHN) noted that, “as nurses, we know the impact of trauma during childhood has lifelong effects” and concluded that “the conditions these children are kept in is abominable and we encourage all nurses to take action against this humanitarian crisis”. The National Association of Pediatric Nurse Practitioners (NAPNAP) called for “immediate action to initiate an investigation of the safety of and conditions in detention facilities”:
“Based on the tragic experience of the last eight months, NAPNAP fears that the conditions under which children and minors are being held in these detention facilities will lead to irreparable physical and mental harm, traumatic injuries and more needless and preventable deaths.”
Physicians ring the alarm: “the smell of sweat and soiled clothing filled the room”
Other healthcare professionals are speaking out as well, collectively and individually, sometimes openly and sometimes anonymously. “Medical providers are challenging practices — by both government agencies and their own hospitals — that they say are endangering patients,” the New York Times reported in June. Physicians said, for example, “that they have been prevented from informing family members about the status of critically ill patients,” and unable to secure the needed follow-up care for long-term detainees with health problems.
Last year already, the American Academy of Pediatrics (AAP), which represents 67,000 pediatricians released a statement which reiterated its position that “immigrant children seeking safe haven in the United States should never be placed in detention facilities”. It cited evidence that children and parents are liable to suffer from depression and posttraumatic stress disorder when held in conditions that have included “forcing children to sleep on cement floors, open toilets, constant light exposure, insufficient food and water, no bathing facilities, and extremely cold temperatures”.
“No child should ever have to endure these conditions,” AAP President Colleen Kraft, MD, concluded, reminding the government that “Alternatives to detention exist. Children and families should have access to legal counsel throughout the immigration pathway and community-based case management can increase the likelihood of compliance with government requirements”.

In July, The Atlantic reported how Dolly Lucio Sevier, MD, a pediatrician from Brownsville, did her best to examine some of the 1,000 migrant children in a Border Patrol warehouse in McAllen, TX, on one mid-June day. That’s the facility where attorneys previously discovered a prematurely born 1-month-old girl who was lethargic, cold, and not eating.
Not having been allowed to enter the cages where the families were being held to find the sickest kids first, Sevier methodically went through a 50-page printout to identify the youngest detainees — the babies and the toddlers. She “saw a baby who’d been fed from the same unwashed bottle for days; children showing signs of malnutrition and dehydration; and several kids who… were exhibiting clear evidence of psychological trauma”:
“As agents brought in the children she requested, Sevier said, the smell of sweat and soiled clothing filled the room. They had not been allowed to bathe or change since crossing the Rio Grande and turning themselves over to officials. Sevier found that about two-thirds of the kids she examined had symptoms of respiratory infection. The guards wore surgical masks, but the detainees breathed the air unfiltered. As the children filed in, Sevier said she found evidence of sleep deprivation, dehydration, and malnutrition too. […]
Each of the agent stations had its own bottle of hand sanitizer and disinfectant wipes. But when Sevier asked the 38 children she examined that day about sanitation, they all said they weren’t allowed to wash their hands or brush their teeth. […]
A 17-year-old girl … entered the room carrying a green plastic bundle—her four-month-old son, wrapped in the kind of bed pad used for incontinent patients in a hospital. The mother explained that the boy had had diarrhea for several days and had soiled his clothes. Guards declined to provide clean baby clothes … so she managed to obtain two extra diapers and flatten them out into rectangles—one for the baby’s back, one for his chest. She had connected them like a disposable tunic, then wrapped him in the plastic pad. … “I carry my baby super close to me to keep his little body warm,” the mother [explained] … Inside the package, the baby was dirty and sticky, Sevier said.”
Sevier discovered two infants with acute respiratory distress, and a total of five infants were admitted to the NICU at a local hospital after her visit. She found that “breastfeeding mothers detained by US Border Patrol are only receiving half the amount of water they need, and hungry babies are not getting enough food,” Buzzfeed News reported: “many infants and children are losing weight” as “some babies were not provided with formula at all and others were not given enough”.

“The source of illness in a facility like Ursula is largely the facility itself”
Some of the young migrants were already sick when they arrived at the border, and most were already traumatized from the dangers they were fleeing. Most young asylum seekers “reported having experienced physical violence, and nearly one out of five said they had suffered sexual violence,” a Physicians for Human Rights report found, chronicling physical injuries and evidence of post-traumatic stress syndrome.
Nevertheless, “the filth, sleep deprivation, cold, and ‘toxic stress’” in the detainee centers and camps are making things immeasurably worse, Julie Linton observed. She co-chairs the American Academy of Pediatrics Immigrant Health Special Interest Group, and concludes that “the source of illness in a facility like Ursula is largely the facility itself”.
Her observations echoed the warnings in a report by the Inspector General of the Department of Homeland Security itself, which examined “five separate Border Patrol facilities” and found “dangerous overcrowding and prolonged detention of children and adults” described by one senior manager as “a ticking time bomb,” which included a facility where people “were held in standing room only conditions for a week” and one where people “were held more than a month in overcrowded cells”.

Federal authorities and local representatives stress that many of the disturbing conditions that are being uncovered now are the tragic, yet inevitable reflection of surging numbers of arrivals. The number of migrants being apprehended by Border Patrol in the Rio Grande Valley rose from almost 100,000 in eight months in 2018 to almost 250,000 in the same period this year. The number of families arriving increased especially steeply, by 269%. There just isn’t enough space to provide adequate shelter to record numbers of Central American immigrant families arriving at the border, authorities argue, and Border Patrol facilities are simply not well equipped to handle children.
The division chief of the Border Patrol’s Laredo sector, Greg Burwell, stressed that “we’ve already [seen] taxpayer dollars to the tune of nearly $10 million go to doctors’ care”. The reality, his colleague Joel Martinez insisted to conservative news site The Daily Signal, “is that agents are providing medical attention.. Daily, our agents save somebody’s life.”
“We have 125 agents out there, at any time, patrolling the streets. And they’re all either paramedics or EMTs.. our guys are usually the first people that render first aid, that actually give IVs and everything else.. Are bad things going to happen? Are we going to lose somebody? Unfortunately, that’s inevitable when you’re dealing with the kind of numbers that we’re dealing with right now. It’s just we’re overwhelmed.”
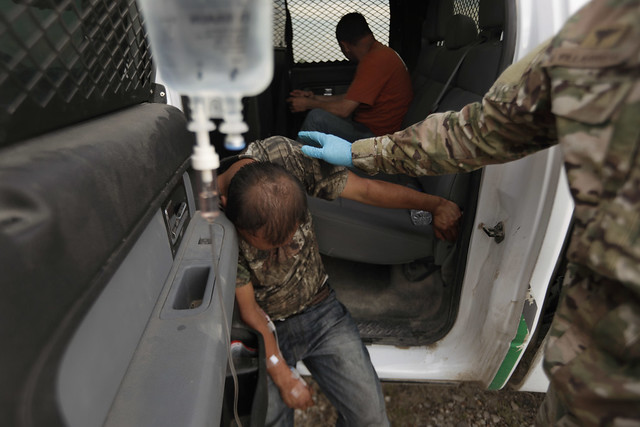
A Customs and Border Protection (CBP) official denied “allegations that children didn’t have access to food, showers and necessities,” explaining that Border Patrol stations designed over 15 years ago lacked showers but shower trailers had been taken to the site and “children can shower at least every three days”.
His claim that “they provide snacks and hot meals including burritos and ramen noodles” to detainees, however, finds a rather different echo in the testimonies which RNRN nurse volunteers passed on:
“Some migrants said they were offered uncooked frozen burritos once a day, but they were not warmed, just left out on a table to thaw. Others told the nurses they were given one or two crackers per person a day, and that parents would give children their own rations.”
“They’re just going to end up getting sick again”: Nurses flag a cycle of illness and trauma
The health hazards children in these conditions face are long-term and structural. Although minors can legally only be held in a facility like the one at McAllen, TX, for 72 hours, “some had been there almost a month”. At the Clint Border Patrol station, around 250 children were moved out after media reported on the conditions there, “but 100 were moved back because there wasn’t room in HHS shelters”. Too many of the children ended up in these facilities after being separated from their parents or guardians. The resulting trauma and deprivation is heartrendingly captured in video footage that was played during a Judiciary Committee hearing into family separation in Congress on July 25:
‘Do you know any 3-year-olds that are criminal or national security threats?’ — This rep had Border Patrol officials watch powerful footage of what the separation policy is doing to real families pic.twitter.com/b7j4mMhojr
— NowThis Impact (@nowthisimpact) July 30, 2019
While the New York Times reported that the individual Border Patrol agents who are tasked with taking ill detainees to hospitals are typically kind and respectful, nurses and physicians saw very different behavior too, and witnessed the harmful consequences of the practices and policies they follow.
Two nurses who spoke anonymously to Buzzfeed News because they feared losing their jobs said that immigration agents were delaying “taking sick children in increasingly dire condition” to their Rio Grande Valley hospital for so long that “many of the children entering the hospital from CBP custody… suffered severe respiratory distress, dehydration, and fevers”. The youngest child they brought in, a one-month-old, had to be rushed to the intensive care unit, one of the nurses said: “I thought, ‘this kid is going to die'”.
Recounting how children “arrived at the hospital with severe diaper rashes because their parents were unable to get clean diapers in CBP custody” and how one kind Border Patrol agent had “asked hospital staff if a girl with a broken arm could stay an extra night because she was still in pain and would otherwise have to sleep on a concrete floor at the station,” the nurses bemoaned the hopeless cycle they faced. “We send them out healthy, but they’re just going to end up getting sick again because they’re going back to the same conditions”.
“People are coming from terrible situations, and a lot of time, hospital policies worsen the situation”
At least some of the responsibility lies with unclear or actively harmful hospital policies, say concerned nurses and physicians. “So many of these situations are occurring where there are no clear guidelines,” a Banner Health employee told Rewire.News, “where we’re not clear on what we can tell Border Patrol to do and not do. It’s unclear what our rights are… It’s creating this atmosphere where health-care providers feel afraid to do the right thing… People are coming from terrible situations, and a lot of time, hospital policies worsen the situation”.
Banner makes no distinction in how it treats immigration detainees (including newly arrived asylum seekers) and prisoners, the New York Times report noted. “It disallows bathroom privileges, requires at least two limbs to be secured to beds unless medically inadvisable, [and] gives agents discretion over whether mothers may visit newborns”.

The results can be dramatic, a case in Texas last year showed. “A cancer patient was admitted to a public hospital accompanied by two guards from the GEO Group, the private contractor for the immigration detention facility where he was being held. [The patient] feared speaking in the earshot of the guards, who, unlike local police officers, refused to step outside during examinations. As the man lay shackled to his hospital bed by both wrists and ankles and at his waist, the skin on his back began to ulcerate. Doctors said they felt intimidated and powerless.”
More specifically, doctors are flagging the impossible position they’re being put in, as Rewire.News chronicled in its thoughtful investigation of the ethical dilemmas and professional hazards of working as health care provider in Arizona.
Dr. Samantha Varner, an OB-GYN resident at Banner-University Medical Centre Tucson, recounted how Border Patrol agents regularly bring in “noticeably pregnant women” and then request her to sign a “cleared for detention” letter at the end of the visit, even though detention conditions are dangerous for pregnant people and a Honduran immigrant gave birth to a stillborn in ICE custody in February. Staff at the hospital’s trauma department and emergency room confirmed they were also receiving these requests, even for patients “who were experiencing health emergencies like renal failure.”
“It’s unethical, but it’s also just not smart”: the health care providers who refuse to sign “cleared for detention” letters
Varner mentioned one case in which immigration agents picked up a young pregnant woman near the border who was dehydrated and in labor, and brought her to Varner’s hospital. When she was ready to discharge the woman two days after safely delivering her baby, they asked her to write a cleared for detention letter. “I thought, ‘Are you insane?’… It’s unethical, but it’s also just not smart. What if she had a delayed postpartum hemorrhage in detention and she bleeds to death, and I’m the OB-GYN who cleared her for detention? I was so shocked they even asked.”
Varner’s apprehension might be justified, a health-care provider at a migrant shelter in the state told Rewire. Her feeling was that “immigration agencies are trying to obtain these letters for legal reasons, to absolve themselves of responsibility should a detained person become gravely ill or die in custody. Responsibility could then be placed on the doctor who put it in writing that the person was “fit” to be detained.”

Varner wasn’t having it, but every time she refused to write the letter, she would face a “battle”. Border Patrol was putting doctors “in a situation of dual loyalty,” Varner argued, “but my loyalty is not with Border Patrol. My loyalty is with my patients and their health”.
Eventually her department drew up an alternative letter with the hospital’s legal team which explicitly says it “should not be construed as any form of approval for detention”. But other doctors have no such hesitations. In one case a doctor even cleared a pregnant patient for detention who had a benign tumor removed, and was in such a weak state that even ICE in the end decided to let her stay in a shelter for longer.
One of Varner’s colleagues, Dr. Justin Gamez, told the New York Times about the time he “refused to certify that a patient was safe to be transported by Border Patrol agents,” only to have an official call him and list the other hospitals he could just take the patient to, who’d willingly write him a letter.
A Physicians for Human Rights report which delves more broadly into the conflicting priorities of immigration enforcement and medical care, Not in My Exam Room, echoes the concern: “Immigration enforcement actions… are putting increasing pressure on medical professionals to compromise patient care”.
Among the examples the report mentions are those of a 10-year-old with cerebral palsy in need of emergency gallbladder surgery, who was arrested while being transferred by ambulance between two hospitals; a patient with metastatic cancer who was only expected to live a few more weeks, whose doctor couldn’t adequately examine him because the detention officers refused to remove his restraints; and reports that immigration authorities were increasingly using information unaccompanied children shared in therapy sessions with mental health professionals against them as evidence in court hearings.
Nurse blogger voices: “I cannot abide”
Time after time, nurse blogger Robin Cogan has spoken up about the crisis at the border and the treatment of migrants and asylum-seekers on her website The Relentless School Nurse. For her, it’s personal. Many of the children in her school have faced the same traumas, she recounted; the same long struggle fleeing from violence or oppression only to get entangled in the webs of US bureaucracy and left without even basic resources:
“Those who judge the families that come to this country seeking asylum may have never been in the desperate position to try to save your children from lawlessness, danger, rape, human trafficking, death, and despair. This is not hyperbole, these are stories that I have heard through my families in Camden.”
“Y’all. I cannot abide”, the bloggers at Radical Nurses wrote. “Children.. are being interned in camps, sleeping on concrete floors, denied access to their parents, caring for babies younger than themselves … This is not congruent with our code of ethics or our professional obligations as nurses.”
Alice Benjamin, who blogs as Nurse Alice, had a chance to take a different approach when she appeared on KTLA 5 News Los Angeles to talk about the five children who had died within five months in the custody of the US Border Patrol. As the interviewer pointed out, “we hear about statistics often, and it’s easy to forget these are individual human beings who are dying, children who are dying”. So Alice reviewed the stories of each one, explaining to the viewers what they died from and what was done to save them.
The stories varied greatly, ranging from one where everyone seems to have done what they could do, as soon as they could do it, to several where something clearly seems to have gone wrong. The case of 7-year old Jakelin Caal Maquin stands out:
“This is a young lady who had to have presented with severe symptoms. When she finally got medical attention, her fever was 105.7 degrees, she had seizures, vomiting, difficulty breathing… she went into cardiac arrest twice before being air-flighted to a children’s hospital.”
Reviewing the five stories, Alice concluded that “I’m really going to encourage the Border Patrol to put some systems in place, and staffing in proportion to the amount of people that are there. You can’t just have one nurse and treat.. thousands. You’re going to need trained professionals, you’re going to need medical equipment, and we’re going to need to act: rather be proactive and save a life than not reactive enough and another child dies – unacceptable.”
https://twitter.com/josephineensign/status/1146222685392736256
Other nurse bloggers responded to news stories about the conditions at the border on Twitter. Josephine Ensign (Medical Margins) called reports about the squalid conditions in border centers “disgusting and immoral”, adding that “this is so un-American and inhuman it has to be stopped”. Barbara C Phillips (Nurse Practitioner Business Owner) tweeted that “as a parent, as a nurse practitioner, as a human being….this is NOT okay!!!” Diana Mason (HealthCetera) tweeted to denounce the separation of children and their parents at the border as “cruel and insane”.
Aid or advocacy? How nurses are trying to help
Identifying concrete ways to make a difference is harder, though — hard enough that some have taken to quilting as act of symbolic solidarity. “There are national groups of healthcare professionals speaking out, raising their voices in outrage at the barbaric treatment of children and families,” Cogan lamented, “but outrage is not a strategy!”
“Nurses are four million strong and together, we can make [an] impact,” Radical Nurses insisted nevertheless. Taking one step closer to home from Cogan’s plea to “vote, march in protest, call Congress.. don’t let the phone stop ringing,” they pointed to a template devised by nurse blogger Death Nurse for holding health care and nursing organisations to account. “Pick five orgs. Contact them. Figure out where they stand on this issue. … Then grade them based on their support of the cause.”

Those who balk at a strategy that relies on scolding organisations by issuing failing grades might feel the urge to go directly to the border to donate basic necessities or offer their own services. Retired nurse Beverly Lyne, for example, was so affected by hearing about two young children who died while in US border custody that she travelled to the border to help migrant families there. She joined the human rights group Border Angels to hand out supplies and offer medical care when she could.
Patricia J. Kelly, a retired professor of nursing and APHAPHN member, volunteered at length in Tucson, AZ, and wrote up her first-hand account of the experience for the American Journal of Nurses (AJN). She also spoke about it with AJN editor-in-chief Shawn Kennedy on its Behind the Article podcast. Patricia started off bringing rice and beans to newly arrived migrant families, facing scepticism about whether she could help without speaking Spanish fluently; but within days she was taking a sick 3-year old child to the ER – on New Year’s Eve, even.
The migrants she worked with had been released by ICE, but owned little but the clothes on their back they’d been wearing for weeks, and had no resources to move on or info about how to. That’s where volunteers step in, she explained. One of their priorities is to conduct a medical screening: “ICE does something, but it seems very erratic.. So what we’re looking for are diseases that they could transmit to other people, say.. scabies or lice, and then.. something that is much more contagious to the community, like chicken pox”. In addition, she added, “their medicines get taken away from them, they’re not allowed to bring in medicines from other countries… So we have found people who were on epilepsy medicine, anti-seizure medicine, who haven’t had any several weeks.”

There are nurses like them on the other side of the border too. Retired nurse Peg Bowden, author of A Land of Hard Edges: Serving the Front Lines of the Border, has been volunteering in towns like Nogales for years. Francisco “Panchito” Olachea, a 57-year-old who was deported to Mexico from the United States himself, now spends all his time “as a volunteer nurse, driving a van he converted into a makeshift ambulance or walking with supplies in his backpack,” Nurse.org reported in a piece that also lists some practical ways for nurses to help migrant families more generally.
Americans who responded to the harrowing news stories by heading directly to the overcrowded detention centers near the border, however, ran into a brick wall. Just because you want to help, they found out, doesn’t mean you can. When a local resident called Austin Savage “heard about the migrant children who said they didn’t have toothbrushes, soap or enough to eat at a nearby Border Patrol station,” for example, he “loaded up a van full of toiletries, diapers and other supplies and drove to the facility in Clint, Texas”. But he was rebuffed, twice. The agents at the station refused to even speak to him.
There were others like him too, the Texas Tribune reported, who attempted to bring things like diapers, bars of soap or toothbrushes, only to find out that you can’t just donate things to the government. Rules and regulations prevent it, a former CBP policy advisor explained, though one official told reporters that they were working to determine “whether Border Patrol stations can legally accept donations”. Texas representatives from both sides of the aisle have introduced bills in Congress to allow Border Patrol to accept donations for children.

“Nurses know”: Keen to help when duty calls
“As the number of refugees and migrants increases” worldwide, the International Council of Nurses (ICN) declared in June, “so does the role of nurses,” who “are at the front line”. Health is a human right, argued ICN President Annette Kennedy, and “nurses play a central role in addressing the physical and mental health challenges of refugees and migrants”.
That puts a special responsibility on nurses, but also on the authorities to consult nurses wherever possible, and on employers and institutions to support them. Governments and the WHO should involve nurses “in the planning, implementation and evaluation of strategies and to promote refugee and migrant health,” the ICN argued at the 72nd World Health Assembly. But “nurses must be supported through education, ongoing training and with adequate resources”.
The ICN also provided some guidance in Health of Migrants, Refugees and Displaced Persons (MRDPs). It calls on nurses to not just “provide ethical, respectful, culturally sensitive and dignified care,” but to develop their own cultural competence and that of the organisations they work in; help migrants and refugees navigate the health system of their new country to find access to the health care services they need; and support organisations that advocate for the healthcare needs of migrants and refugees.

It’s a call of duty, both main nursing organisations in the US agree. “As nurses, we have a duty through the Code of Ethics for Nurses to speak out and advocate for the human rights and health care needs of all, particularly the most vulnerable,” the ANA’s Brooke Trainum and Janet Haebler wrote. “As nurses, we have a moral obligation to demand that our government.. provide them with the medical care they need and deserve,” is how NNU executive director Bonnie Castillo put it.
“Nurses know,” she says. “Nurses know that when we tear children from their mothers, their fathers, their sisters, brothers… and throw them into cold cages, without adequate food, water, or the support of an adult, we are causing harm, and lasting trauma. We are failing to uphold basic human rights when we refuse to provide the bare minimum to keep a scared child warm, fed, and safe.”
“There can be no keener revelation of a society’s soul than the way in which it treats its children,” Cogan quoted Nelson Mandela. “Like many school nurses,” she admitted, “I struggle with how to help the families navigate the treacherous waters of a seemingly unwelcoming country.” But “kindness, listening and observing, are tools that we all possess and they are freely available”; and our schools can be trauma-responsive “beacons of light for families who are struggling”. We have no choice, she argues, but to “stand up for children, no matter how they have arrived in our country,” because “they deserve the best of who we are, not the worst”.
Look at my students, many of their families sought asylum at the same border crossings where families have been separated. #FlatLillian visited us this week. Caring for immigrant children is a privilege. Meet your future leaders, care about them, they need it!@HenryStreet pic.twitter.com/ZjSvstOjyQ
— @robincogan.bsky.social 🟧 (@RobinCogan) March 17, 2019
That’s the spirit in which Patricia Kelly and Maria Rojas volunteered their nursing expertise at the border too. Currently, the “health volunteer pool is.. a little shallow,” warns Kelly, even with the RNRN volunteers joining for weekends “to stretch [it] further,” so she is trying “to get more volunteers here”:
“I would like nurses to understand that they can be involved, and that it is just a wonderful opportunity.. This is not heavy medical, this is screening, compassion, respect, and this is something that all nurses know how to do. And the more of us that are there, the better it is both for these families coming through, and the better it is for nursing.”
Maria captured that same spirit in just a few, moving words:
It is just a blessing I have health and knowledge to help others and make their lives a little bit better and that is why I went into nursing, just being there to hold their hand and listen, that is how I get fulfillment.

Donna C. Neil-Demir
I am so offended in every way it is difficult to find words. I am a R.N which means I have a particular skill set with which I can save a life but I’m a human being first. This hurts my heart. How can any human being do this or agree to this? I know how, by being evil and lacking an awareness of God Almighty himself. America is in big trouble as we’ve lost our soul.
Dr Bonnie Arzuaga on behalf of D4CC
Hi!
I’ve been feeling like I want to “do something” about what’s going on at the border.
On July 30th, I started a grassroots effort called Doctors for Camp Closure (open to all healthcare clinicians). We currently have over 1300 physician members as well as many other members who are nurses, social workers, PhDs, etc. Please consider attending our March for Migrants on October 19th, and signing up to volunteer for the event:
https://d4cc.squarespace.com/volunteer-signup
If you can’t volunteer but want to stay informed, you can get more information and sign up for our mailing list at:
https://d4cc.squarespace.com/
https://www.facebook.com/events/502689727208848/
If you are interested in lobbying with us on October 18th, please sign-up at https://docs.google.com/forms/d/e/1FAIpQLSfOfm-yAqh8b5A7ruj4WeygEEs3oyYgiuLKhO6BSl0PRzwPKg/viewform?usp=sf_link
Please share this information with your networks!
Kim collins
How can a nurse sign up to be deployed to work at the boarder? I would like to join this organization.